Health
obstetrika: The Living Science of Birth and Care
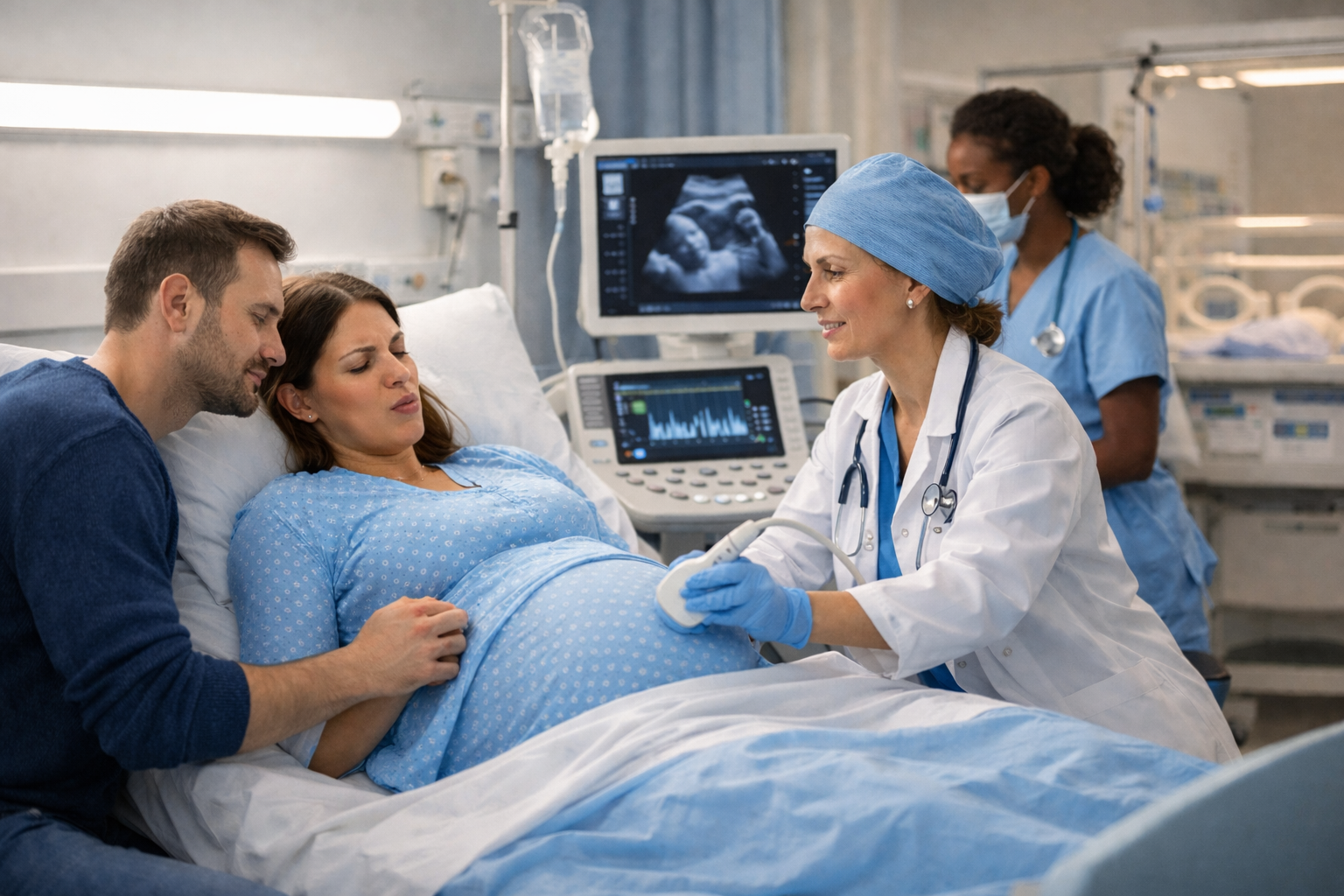
Introduction
Childbirth is one of the most profound and transformative events in human life. It is a moment where biology, emotion, risk, science, and hope intersect. Across centuries and civilizations, the act of bringing new life into the world has shaped societies, cultures, and medical progress itself. Today, the discipline that carefully guides this journey from conception to delivery is known as obstetrika.
More than a branch of medicine, obstetrika represents a living science—one that evolves constantly in response to new discoveries, technological advancements, and shifting understandings of maternal and fetal health. It exists at the crossroads of compassion and clinical precision. Every decision made within this field carries weight not only for the mother, but also for the unborn child and, in many ways, for the future itself.
To understand obstetrika fully, one must look beyond hospital walls. It is rooted in ancient traditions, strengthened by modern research, and shaped daily by real human stories. This article explores its meaning, scope, evolution, challenges, and significance in a world where safe motherhood remains both a triumph and a challenge.
What Is obstetrika
Obstetrika is the medical discipline focused on pregnancy, childbirth, and the postpartum period. It encompasses the monitoring of maternal health, the development and wellbeing of the fetus, the management of labor, and the care provided after delivery. While often closely associated with gynecology, obstetrika has its own distinct scope centered specifically on reproductive events surrounding birth.
The field includes both normal physiological pregnancies and high-risk situations that require advanced medical intervention. Conditions such as preeclampsia, gestational diabetes, placental abnormalities, premature labor, and fetal growth restriction fall within its domain. Practitioners trained in obstetrika are responsible for recognizing early warning signs, making timely decisions, and balancing safety with natural processes.
Unlike many medical specialties that treat disease alone, obstetrika deals primarily with a natural biological function. Yet, this natural process can quickly shift into a life-threatening emergency if not managed properly. That delicate balance between supporting nature and intervening when necessary defines the essence of obstetrika.
The Historical Roots of obstetrika
Long before modern hospitals existed, childbirth was guided by midwives and traditional healers. Ancient civilizations in Egypt, Greece, India, and China developed early knowledge about pregnancy and labor, though it was often mixed with superstition. For centuries, birth took place at home, attended by experienced women within the community.
The scientific transformation of obstetrika began during the Renaissance and accelerated in the nineteenth century. The introduction of antiseptic techniques dramatically reduced maternal deaths caused by infection. Anesthesia changed the experience of labor. The invention of forceps provided assistance during difficult deliveries. Later, the development of cesarean section as a safer surgical procedure marked another turning point.
In the twentieth century, ultrasound imaging revolutionized obstetrika by allowing physicians to visualize fetal development in real time. This shifted prenatal care from guesswork to measurable monitoring. Modern genetics, fetal surgery, and neonatal intensive care further expanded the scope of what is possible. What began as community-based support has become a highly specialized medical field grounded in research and technology.
The Scope of obstetrika in Modern Medicine
Today, obstetrika covers the entire continuum from preconception counseling to postpartum recovery. The journey typically begins before pregnancy itself, when medical professionals evaluate overall health, nutritional status, and risk factors that may affect future pregnancies.
During pregnancy, regular prenatal visits assess blood pressure, fetal growth, maternal weight, and laboratory markers. Imaging technologies track organ development and detect structural abnormalities. Screening tools identify chromosomal conditions. These measures aim not only to treat complications but to prevent them.
Labor management forms another central pillar. Decisions regarding induction, pain management, monitoring fetal heart rate, and determining the mode of delivery fall under obstetrika. In complicated cases, emergency surgical intervention may be required within minutes. Precision and preparedness are essential.
The postpartum period, often underestimated, is equally critical. Hemorrhage, infection, mood disorders, and breastfeeding challenges require careful attention. Obstetrika recognizes that childbirth does not end with delivery; recovery and adjustment are part of the medical responsibility.
Technology and Innovation in obstetrika
Technological progress has dramatically reshaped obstetrika. Ultrasound imaging now provides detailed 3D and even 4D visualization of fetal anatomy. Doppler studies measure blood flow in placental vessels, helping detect fetal distress early.
Electronic fetal monitoring continuously tracks heart rate patterns during labor, offering clues about oxygen supply. Minimally invasive fetal procedures can treat certain congenital conditions before birth. In vitro fertilization and assisted reproductive technologies have expanded the boundaries of possibility for families who once faced infertility.
Artificial intelligence is increasingly being studied to predict complications such as preterm birth or hypertensive disorders. While technology enhances accuracy, it also raises ethical questions about intervention thresholds and decision-making autonomy. The human element remains indispensable in obstetrika, even in an age of machines.
The Human Dimension of obstetrika
Despite its scientific rigor, obstetrika is deeply human. Pregnancy is not simply a clinical state; it is a time of anticipation, vulnerability, and emotional intensity. Practitioners must communicate complex medical information while respecting personal values, cultural traditions, and family dynamics.
Every pregnancy carries uncertainty. Even low-risk cases can evolve unpredictably. In high-risk scenarios, difficult conversations about maternal safety or fetal prognosis may arise. Sensitivity and clarity become as important as technical skill.
In many parts of the world, access to skilled obstetric care remains limited. Maternal mortality is still a significant global issue. This reality highlights that obstetrika is not only a hospital specialty but also a public health priority. Training, infrastructure, and equitable access determine whether childbirth becomes a celebration or a tragedy.
Risk Management and Ethical Complexity
Few medical fields involve such high stakes. Decisions made within obstetrika often affect two lives simultaneously. Balancing maternal autonomy with fetal wellbeing can present ethical dilemmas.
For example, when a recommended intervention is declined by a pregnant patient, healthcare providers must navigate respect for personal choice while ensuring informed understanding of risks. In emergency situations, time-sensitive decisions may require swift judgment with limited data.
Additionally, issues surrounding genetic testing and selective intervention challenge moral boundaries. Advances in prenatal diagnosis allow early detection of anomalies, but they also prompt profound ethical considerations about choice, disability, and societal attitudes. Obstetrika operates within these sensitive spaces, requiring not only medical expertise but moral discernment.
Global Perspectives on obstetrika
The practice of obstetrika varies widely across countries. In high-resource settings, routine prenatal visits, advanced imaging, and emergency surgical facilities are standard. In low-resource regions, women may give birth without trained professionals or sterile environments.
International organizations continue to emphasize skilled birth attendance as a cornerstone of maternal safety. Improvements in transportation systems, blood banking, and emergency response protocols have significantly reduced maternal deaths where implemented effectively.
Cultural beliefs also shape experiences of pregnancy and birth. In some societies, childbirth remains deeply communal. In others, it is highly medicalized. Obstetrika must adapt to these diverse realities while maintaining evidence-based standards.
Education and Professional Training
Becoming a specialist in obstetrika requires years of rigorous education. Medical graduates undergo intensive residency training, where they learn to manage both routine deliveries and life-threatening emergencies. Surgical skills, diagnostic interpretation, and patient counseling form the core of this preparation.
Continuous education is essential because guidelines evolve. Research constantly refines best practices in labor induction, cesarean section criteria, medication safety, and neonatal resuscitation. The field demands lifelong learning.
Simulation-based training has gained importance, allowing teams to rehearse rare but critical emergencies such as shoulder dystocia or postpartum hemorrhage. These rehearsals improve coordination and response times, ultimately saving lives.
Psychological and Social Impact
Pregnancy can profoundly influence mental health. Anxiety about fetal wellbeing, fear of labor pain, or past traumatic experiences may shape the journey. Postpartum depression and anxiety disorders require early recognition and intervention.
Obstetrika increasingly acknowledges mental health as an integral component of maternal care. Screening tools and multidisciplinary collaboration with psychologists and social workers have become more common. Addressing emotional wellbeing is not secondary; it directly affects outcomes for both mother and child.
Moreover, societal expectations around motherhood can create pressure. Some women feel judged for their birth choices, whether opting for natural delivery or surgical intervention. A respectful, individualized approach within obstetrika helps reduce stigma and empower informed decisions.
The Future of obstetrika
The future promises further innovation. Advances in genomics may allow earlier prediction of complications. Telemedicine is expanding access to prenatal consultations in remote areas. Wearable health technologies may monitor vital signs continuously during pregnancy.
At the same time, there is a growing movement toward patient-centered care. Women increasingly seek shared decision-making and personalized birth plans. The challenge for obstetrika lies in harmonizing technological progress with respect for autonomy and human experience.
Sustainability and equitable access will also define the coming decades. Reducing disparities in maternal outcomes remains a global goal. The field must address systemic inequalities while continuing scientific advancement.
Conclusion
Obstetrika stands as one of medicine’s most vital and emotionally charged disciplines. It safeguards the beginning of life while navigating unpredictable risks. Rooted in ancient traditions yet propelled by modern science, it reflects both humanity’s vulnerability and its ingenuity.
From prenatal care to postpartum recovery, obstetrika weaves together technology, ethics, compassion, and precision. Its success is measured not only in survival rates but in the dignity, safety, and confidence it provides to mothers and families.
As medical knowledge grows and global awareness deepens, the field will continue to evolve. Yet its central mission remains constant: to ensure that the journey into life is guided with care, respect, and unwavering expertise.
FAQs
What does obstetrika focus on primarily?
Obstetrika focuses on pregnancy, childbirth, and the postpartum period, ensuring the health and safety of both mother and baby throughout these stages.
Is obstetrika different from gynecology?
Yes, obstetrika specifically addresses pregnancy and delivery, while gynecology covers the broader spectrum of women’s reproductive health outside of pregnancy.
Why is prenatal care important in obstetrika?
Prenatal care allows early detection of complications, monitors fetal development, and reduces risks during labor and delivery.
What are common complications managed in obstetrika?
Conditions such as preeclampsia, gestational diabetes, preterm labor, and placental abnormalities are commonly handled within this field.
How is technology changing obstetrika?
Advanced imaging, genetic screening, minimally invasive procedures, and digital monitoring systems are enhancing diagnosis, safety, and personalized care in modern obstetrika.
Health
Choosing the Right Veterinarian Near Addison, TX: What to Ask and Look For

Finding the right vet for your pet can feel a bit like finding the right doctor for yourself. You want someone who not only understands animals but also genuinely cares about them. If you’re searching for a Veterinarian addison TX, you probably already know that choosing the right clinic isn’t just about convenience. It’s about trust, comfort, and knowing your pet is in caring hands.
Let’s go through what really matters when picking a vet in Addison and what to ask before you make your first appointment.
Why Your Choice of Vet Matters
Your vet isn’t just there for vaccinations and checkups. They become a long-term partner in your pet’s health and wellbeing. Whether your pet is dealing with allergies, recovering from surgery, or just needs a dental cleaning, the quality of care makes all the difference.
A good veterinarian takes time to listen to your concerns, explains treatment options clearly, and makes sure you understand how to care for your pet at home. They’ll also help you make informed decisions that fit your pet’s lifestyle, age, and personality.
What to Look for in a Veterinarian
When exploring clinics near Addison, focus on qualities that go beyond the basics.
1. Experience and qualifications: Look for a clinic with experienced staff who have handled different types of animals and conditions. The right Veterinarian addison tx will have up-to-date certifications, use modern technology, and stay informed about new treatment options.
2. Clean and welcoming environment: The atmosphere of a clinic says a lot. When you visit, check if the space feels clean, calm, and well-organized. Pets can pick up on stress, so a peaceful setting helps them relax during visits.
3. Friendly communication: You should feel comfortable asking questions, no matter how small. A great vet will never rush you. They’ll explain medical terms in simple language and make sure you feel confident about your pet’s care.
4. Comprehensive services: Some clinics only handle basic exams, while others provide everything from dental care to surgical treatments and preventive wellness programs. Choosing a clinic with broad services can save you time and give your pet consistent care under one roof.
5. Compassion and patience: This is something you can sense right away. Notice how the staff interacts with animals and owners. A gentle tone, patience with nervous pets, and genuine warmth go a long way in making your visits easier.
Questions to Ask Before Choosing a Vet
Before committing to a clinic, it helps to ask a few key questions:
- What types of pets do you treat most often?
- What are your emergency care options after hours?
- How do you handle anxious or aggressive animals?
- Do you provide regular wellness plans or preventive care packages?
- How do you communicate lab results or follow-up updates?
These questions will give you insight into how the clinic operates and how attentive they are to your pet’s individual needs.
Consider Accessibility and Location
Location may not be the first thing you think about, but it’s important, especially during emergencies. A nearby clinic can make it easier to schedule regular visits and get urgent care quickly if needed. If you live in or around Addison, there are several well-reviewed options that balance convenience and quality care.
Parking availability, office hours, and appointment flexibility are also small details that can make a big difference in the long run.
How to Know When You’ve Found the Right Fit
You’ll know you’ve found the right veterinarian when both you and your pet feel at ease during visits. Your pet’s body language says a lot, relaxed tails, curious sniffs, or calm behavior are good signs that they feel safe.
A strong vet-pet relationship builds over time. Regular checkups, transparent communication, and consistent care help create a bond of trust. When emergencies arise or health issues appear, having a familiar team that already knows your pet’s history makes everything smoother.
Final Thoughts
Choosing the right Veterinarian addison TX is about finding a balance of skill, compassion, and trust. When your vet truly listens, communicates clearly, and treats your pet with respect, you’ll feel confident you made the right choice.
If you’re exploring local options and want a place that understands both medical expertise and emotional care for your furry family member, you can visit Midway Road Animal Clinic. Their team provides friendly, professional support that helps pets live healthier, happier lives and helps owners feel at ease knowing their companions are in good hands.
Health
Wheon.com Health News: Latest Updates

Introduction to Wheon.com Health News
In today’s fast-paced digital world, staying updated with accurate health information has become more important than ever. Whether you’re searching for the latest medical research, nutrition guidance, or wellness hacks, wheon.com health news provides a one-stop solution. With trusted insights and fresh updates, this platform is making a mark in the health and wellness space.
Unlike random blogs or unverified articles circulating online, wheon.com health news delivers content backed by experts, researchers, and healthcare professionals. This makes it a go-to resource for individuals who care about their overall well-being and want practical tips to improve their daily lifestyle.
Why Wheon.com Health News Is Gaining Popularity
Trusted Source for Health Enthusiasts
Readers prefer wheon.com health news because it consistently provides authentic and fact-checked content. With misinformation spreading online, having a reliable source is essential.
Covering All Aspects of Well-being
From physical fitness and mental health to diet trends and medical news, the platform covers everything related to healthy living.
Latest Topics Covered in Wheon.com Health News
Medical Breakthroughs and Research
Readers can explore detailed coverage of new medical studies, FDA approvals, and groundbreaking therapies.
Nutrition and Healthy Eating
Nutrition is at the heart of a healthy lifestyle. Expect practical guides on balanced diets, superfoods, and the truth about trending diets.
Fitness and Exercise Trends
Workout routines, yoga practices, and gym-free fitness hacks are well-explained for both beginners and professionals.
Mental Health Awareness
Articles highlight ways to manage stress, anxiety, and emotional well-being, which are often overlooked in other portals.
Lifestyle and Wellness Hacks
Small but powerful lifestyle changes like better sleep, hydration tips, and posture correction are frequently shared.
Benefits of Reading Wheon.com Health News Regularly
Staying Informed with Reliable Updates
New research and findings are updated frequently, helping readers stay ahead in their health journey.
Expert Opinions You Can Trust
Content is often reviewed or contributed by professionals in the healthcare sector.
Practical Tips for Everyday Health
Instead of heavy medical jargon, the platform offers simple solutions that can be applied daily.
How Wheon.com Health News Helps in Daily Life
Guidance for Families and Parents
Parents get valuable tips on children’s nutrition, immunity, and healthy routines.
Support for Seniors and Elderly Care
The site also focuses on aging gracefully and managing common age-related issues.
Advice for Busy Professionals
Quick health hacks and stress-relief techniques are shared for working individuals.
SEO Impact of Wheon.com Health News in Digital Media
Optimized for Google Algorithm Updates
The platform uses strategies like keyword-rich headlines, schema markup, and E-E-A-T (Experience, Expertise, Authority, Trustworthiness).
Featured Snippets and SERP Techniques
By providing direct answers to common health queries, wheon.com health news often secures top spots in Google snippets.
Comparison: Wheon.com Health News vs Other Health Portals
Unique Features of Wheon.com
The site blends expert analysis with easy-to-read content, unlike many portals that are either too technical or too shallow.
Why Readers Prefer Wheon.com Health News
Its balanced approach, updated articles, and reader-friendly language attract organic traffic.
Tips to Get the Best Out of Wheon.com Health News
Setting Health Goals with Articles
Readers can use guides to set realistic health goals and track progress.
Creating a Daily Reading Habit
Spending even 10 minutes a day on wheon.com health news can help build healthier routines.
❓ FAQs on Wheon.com Health News
Q1: What is Wheon.com Health News?
A reliable online platform providing the latest updates on health, fitness, nutrition, and wellness.
Q2: Is Wheon.com Health News trustworthy?
Yes, articles are fact-checked and often supported by medical professionals.
Q3: Does Wheon.com Health News cover mental health?
Absolutely. It features stress management, mindfulness, and emotional wellness guides.
Q4: Can I find nutrition tips on Wheon.com Health News?
Yes, it shares diet tips, superfoods, and expert-backed nutrition advice.
Q5: How often is Wheon.com Health News updated?
Content is updated regularly with new health discoveries and trending topics.
Q6: Is Wheon.com Health News free to access?
Yes, readers can access health information without any subscription fee.
Conclusion: Why Wheon.com Health News is Your Go-To Health Resource
In a world filled with misinformation, wheon.com health news shines as a trustworthy platform for authentic and practical health updates. Its easy-to-understand content makes it suitable for everyone, from teenagers to senior citizens.
Health
Doge HHS Migrant Housing Contract

Understanding the doge hhs migrant housing contract is essential for anyone tracking federal migrant housing efforts. This article clearly explains the contract’s terms, challenges, and implications while providing actionable takeaways and maintaining SEO-quality balance.
What Is the Doge HHS Migrant Housing Contract?
At its core, the doge hhs migrant housing contract involves a partnership between the Department of Health and Human Services (HHS) and private providers. The goal is to offer temporary housing, essential services, and care for unaccompanied migrant children. Through this agreement, the HHS ensures safety, medical attention, and counseling for minors in federally funded shelters.
Purpose and Objectives
Such contracts serve three main purposes:
- Safety and Shelter – Create stable environments for vulnerable minors.
- Health and Wellness – Provide meals, medical care, and mental health counseling.
- Compliance and Standards – Ensure shelters follow federal guidelines regarding child protection and policy requirements.
Key Terms and Conditions
The agreement includes:
- Payment Structure – Providers receive reimbursement based on daily per-child rates.
- Performance Metrics – Requirements include staff-to-child ratios, background checks, and documentation.
- Reporting Obligations – Regular data reports ensure transparency and federal oversight.
Altogether, these elements aim to protect minors while maintaining accountability.
Stakeholders and Their Roles
- HHS/ORR – Oversees licensing, compliance audits, and contract renewal.
- Private Providers – Manage site operations, staff training, and daily child care.
- Local Authorities – Coordinate services, health inspections, and emergency responses.
Through collaboration, the contract seeks to foster effective delivery of services.
Transparency and Accountability
Contract transparency is vital when public funds are used. Therefore:
- Open Records – Many documents remain accessible under the Freedom of Information Act.
- Performance Dashboards – Data on occupancy rates, expenditures, and staffing is often published online.
- Independent Audits – Regular reviews by oversight bodies hold providers responsible.
Encouraging compliance through public scrutiny strengthens trust in the system.
Risks, Challenges, and Criticisms
Although the contract aims to help, critics highlight concerns:
- Cost Overruns – High daily rates may strain federal budgets, especially during surges.
- Quality Gaps – Some providers may underdeliver due to staff shortages or insufficient training.
- Legal Pushback – Lawsuits sometimes arise over due process, extended stays, or reunification delays.
Addressing these challenges demands continuous improvement and public engagement.
7Recent Developments & Reforms
Recently, several updates have emerged:
- Renewed Contracts – New solicitations emphasize child protections, mental health, and educational support.
- Expanded Oversight – Increased federal audits and inspections aim to close gaps.
- Community Involvement – Local NGOs and advocates partner to enhance service delivery and communication.
Such reforms aim to ensure the doge hhs migrant housing contract remains efficient and humane.
Impact on Migrant Children & Communities
The contract’s effects are profound:
- For Children – Access to housing, meals, medical care, and legal orientation is life-changing and stabilizing.
- For Communities – Local economies benefit from shelter operations and employment opportunities.
- For Federal Goals – Smooth reunification processes and safety compliance help preserve public trust.
These outcomes align with the contract’s core mission of protection and care.
Future Outlook and Recommendations
To improve the contract, stakeholders should:
- Strengthen Outcomes Metrics – Use long-term indicators like reunification success rates.
- Promote Transparency – Expand public access to real-time compliance data.
- Foster Collaboration – Encourage community groups and legal advocates to supplement care and oversight.
With these measures, the doge hhs migrant housing contract can evolve to better serve children and communities.
Conclusion: Ensuring Accountability in the Doge HHS Migrant Housing Contract
Overall, the doge hhs migrant housing contract plays a vital role in safeguarding unaccompanied migrant children. Moreover, when transparency, oversight, and community partnerships are prioritized, this federal program can deliver both compassion and accountability. Public engagement and policy evolution will remain crucial.
Frequently Asked Questions (FAQs)
Q1: What is included in the doge hhs migrant housing contract?
A1: It covers shelter operations, care services, staff standards, reporting, and compliance with child welfare laws under HHS supervision.
Q2: Who oversees these housing providers?
A2: The Office of Refugee Resettlement (ORR) within HHS performs audits, licensing checks, and contract renewals.
Q3: How are providers paid?
A3: They receive daily per-child reimbursements tied to occupancy and performance metrics.
Q4: Can the public access contract details?
A4: Yes. Many parts are available via FOIA, and performance dashboards share data publicly.
Q5: What are common criticisms of the contract?
A5: Critics cite high costs, occasional quality lapses, and legal concerns over detention durations or paperwork errors.




